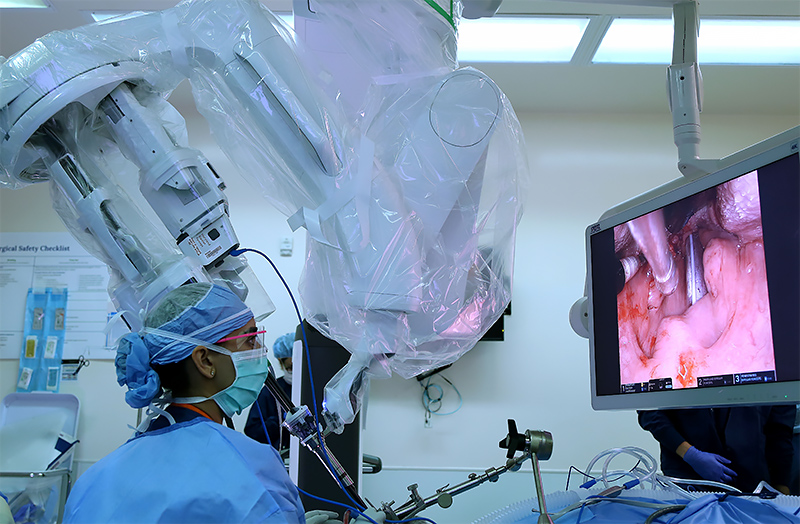
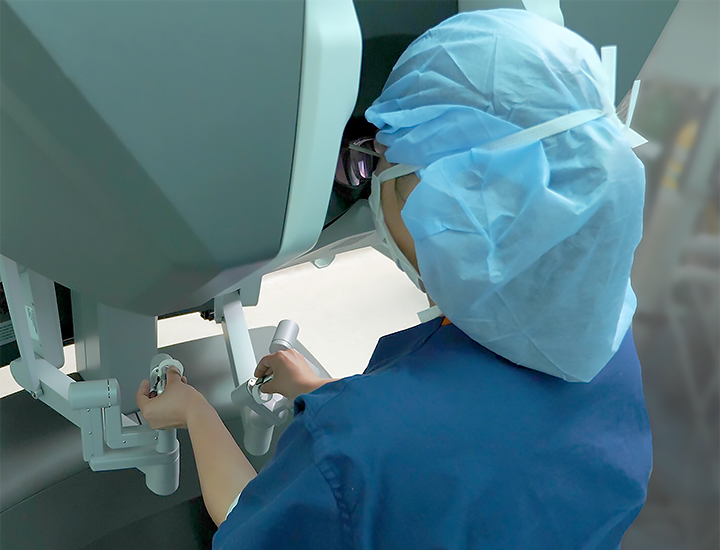
Learn More About TORS
If you have questions about transoral robotic surgery, HPV-related oropharyngeal cancer, or would like an expert second opinion, please call today or use the form to receive a call back, or email.
Call 310-829-8701.

Send us a message.
Use the form below to ask your question. We will respond as soon as possible.